A 72-year-old patient presented with bilateral blurred vision. Best-corrected visual acuity was 0.1 in both eyes.
The patient’s medical history is significant for systemic hypertension, prior stroke, and membranoproliferative glomerulonephritis. Blood creatinine levels were elevated.
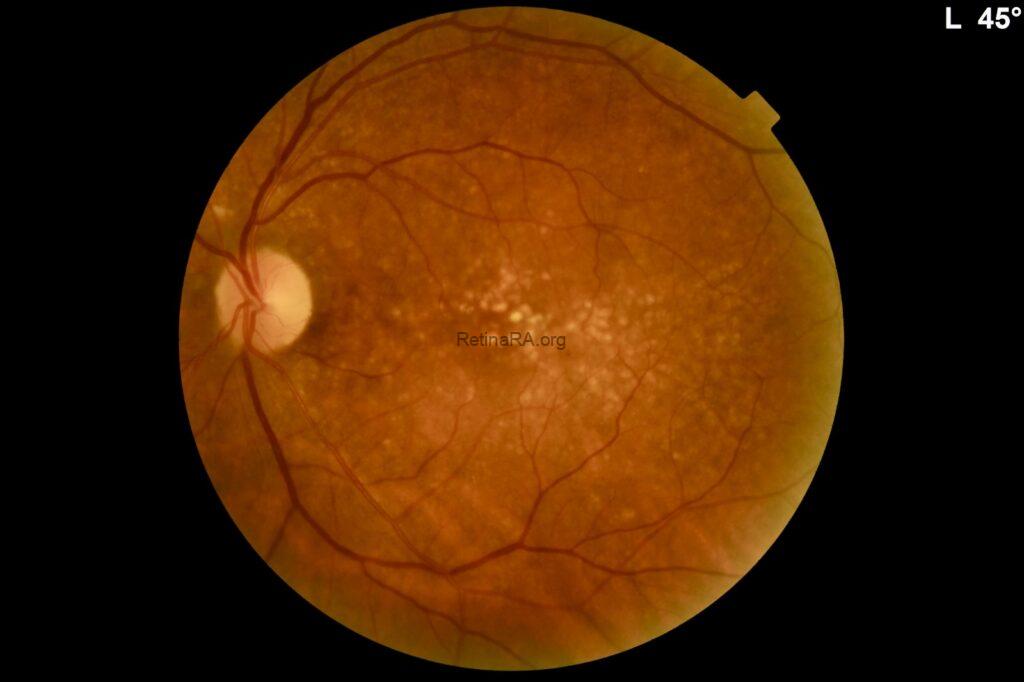
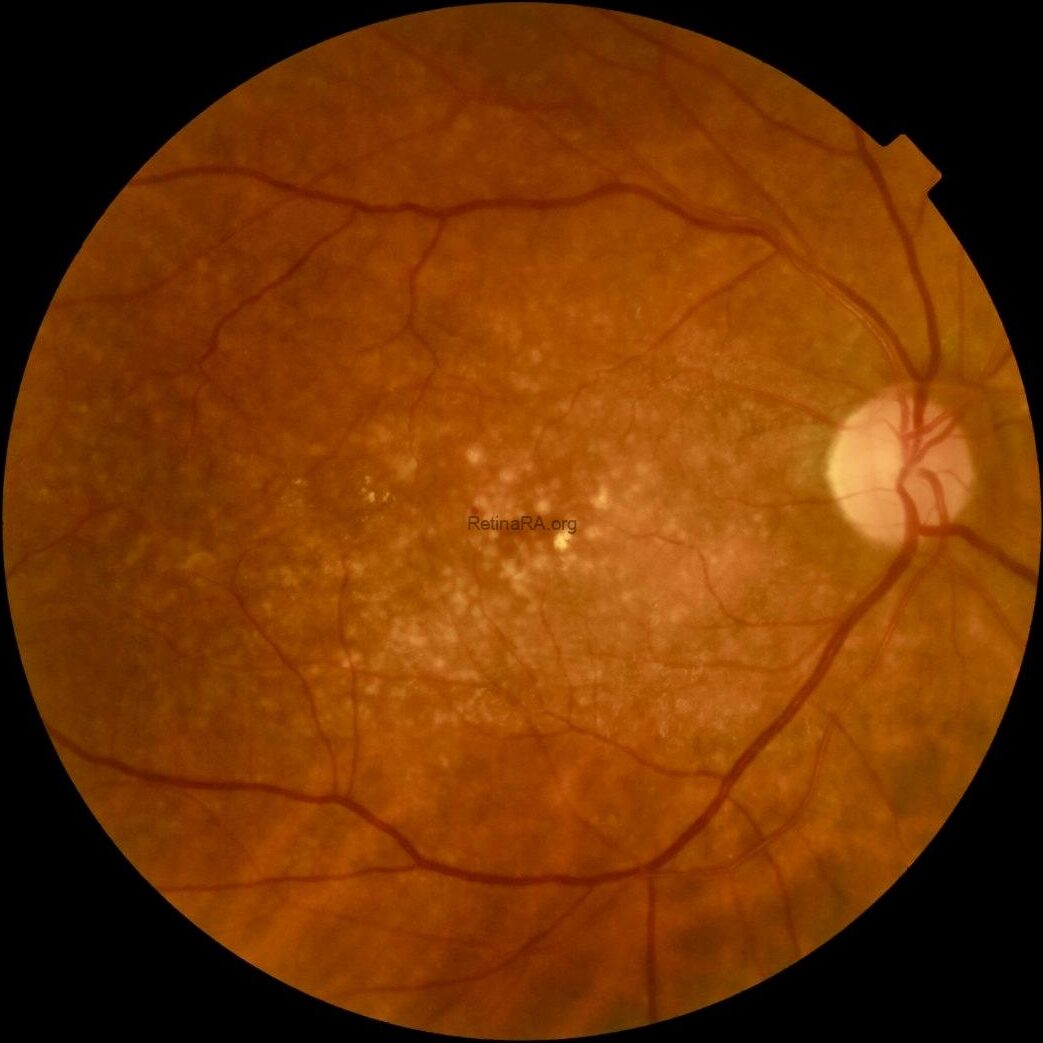
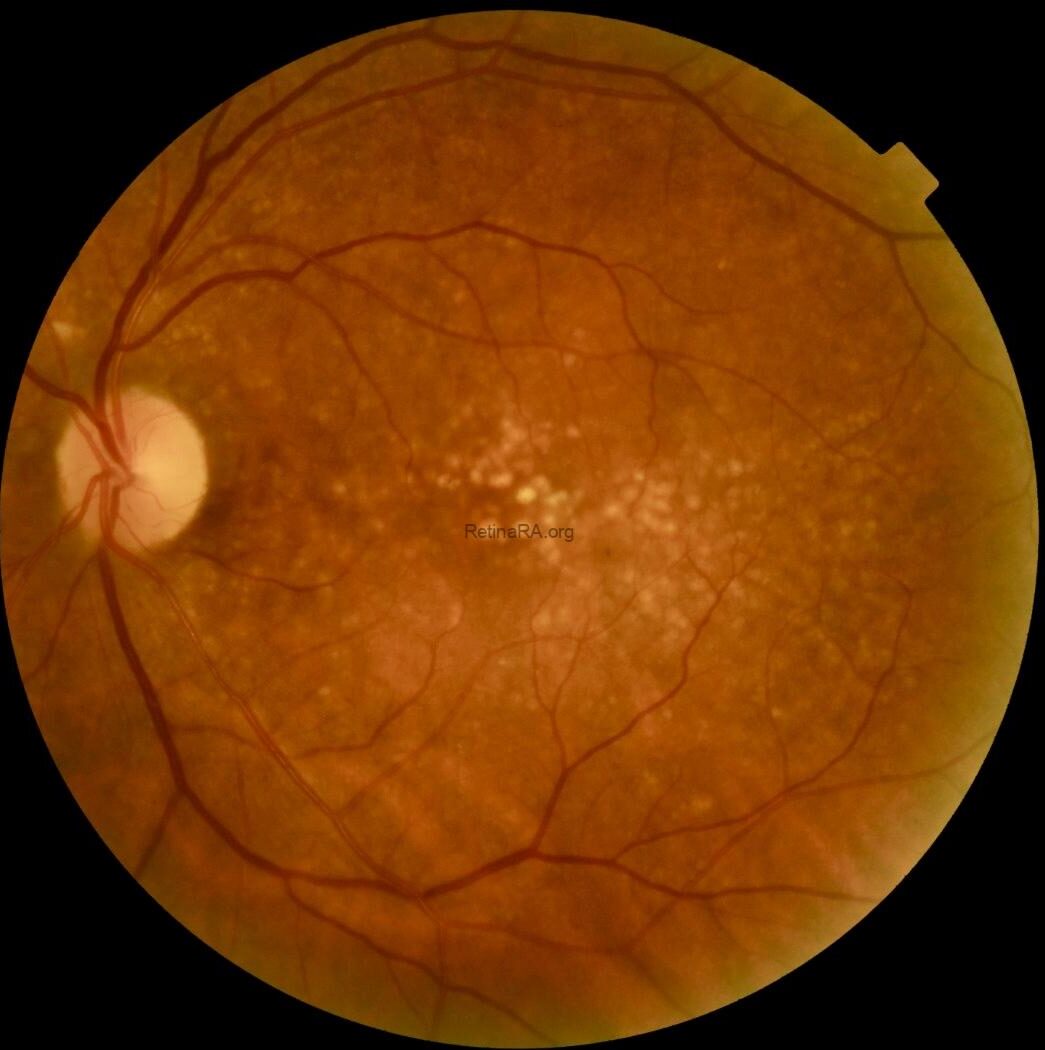
Color fundus photography revealed widespread, yellowish dense deposits involving the macula and extending beyond the macular region in both eyes.
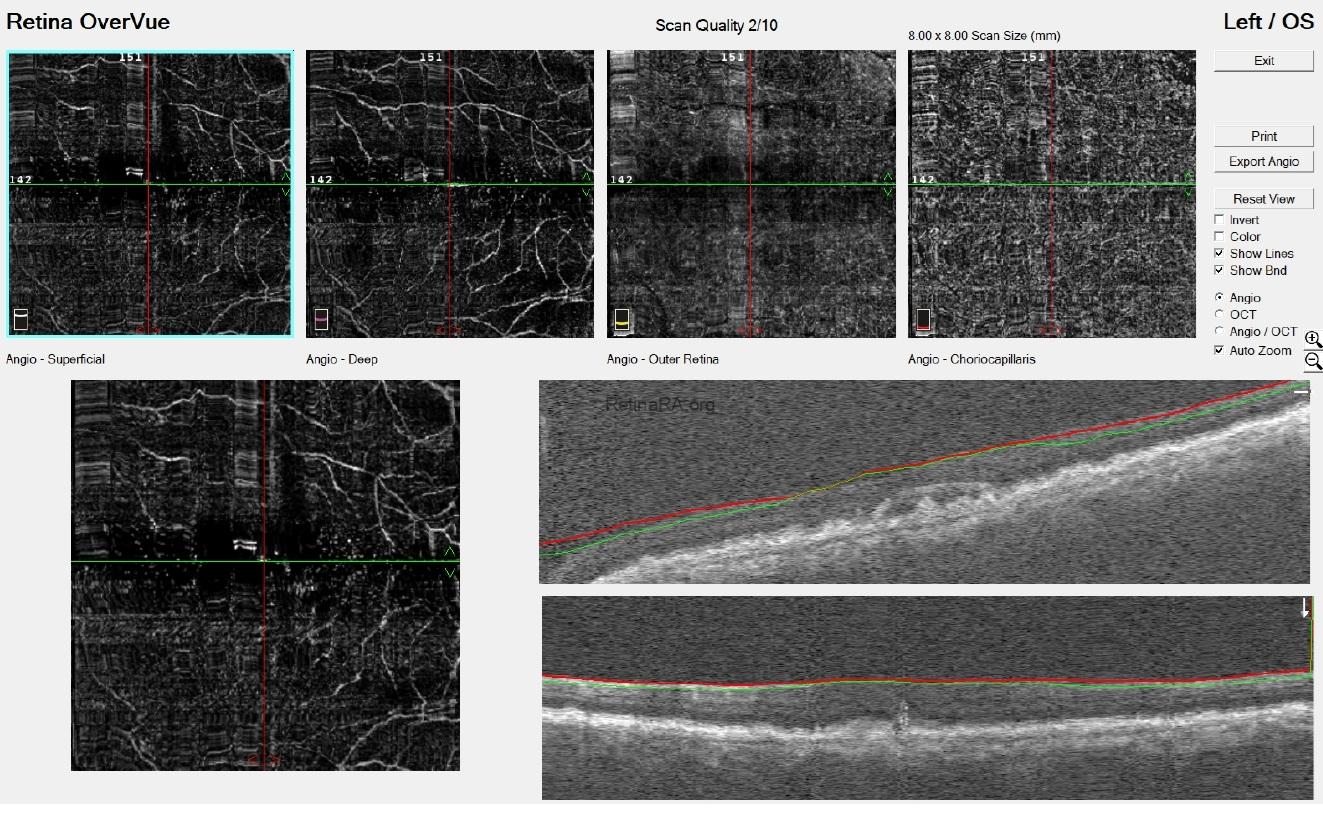
Optical coherence tomography (OCT) demonstrated extensive drusen-like deposits bilaterally, with areas of Bruch’s membrane thickening. In the right eye, there were vitreopapillary traction and an epiretinal membrane associated with a lamellar macular hole configuration, consistent with lamellar hole–associated epiretinal proliferation (LHEP). In the left eye, similarly dense deposits were observed, along with a subtle subfoveal subretinal fluid accumulation. Additionally, there appeared to be localized thickening at the level of the photoreceptor layers.
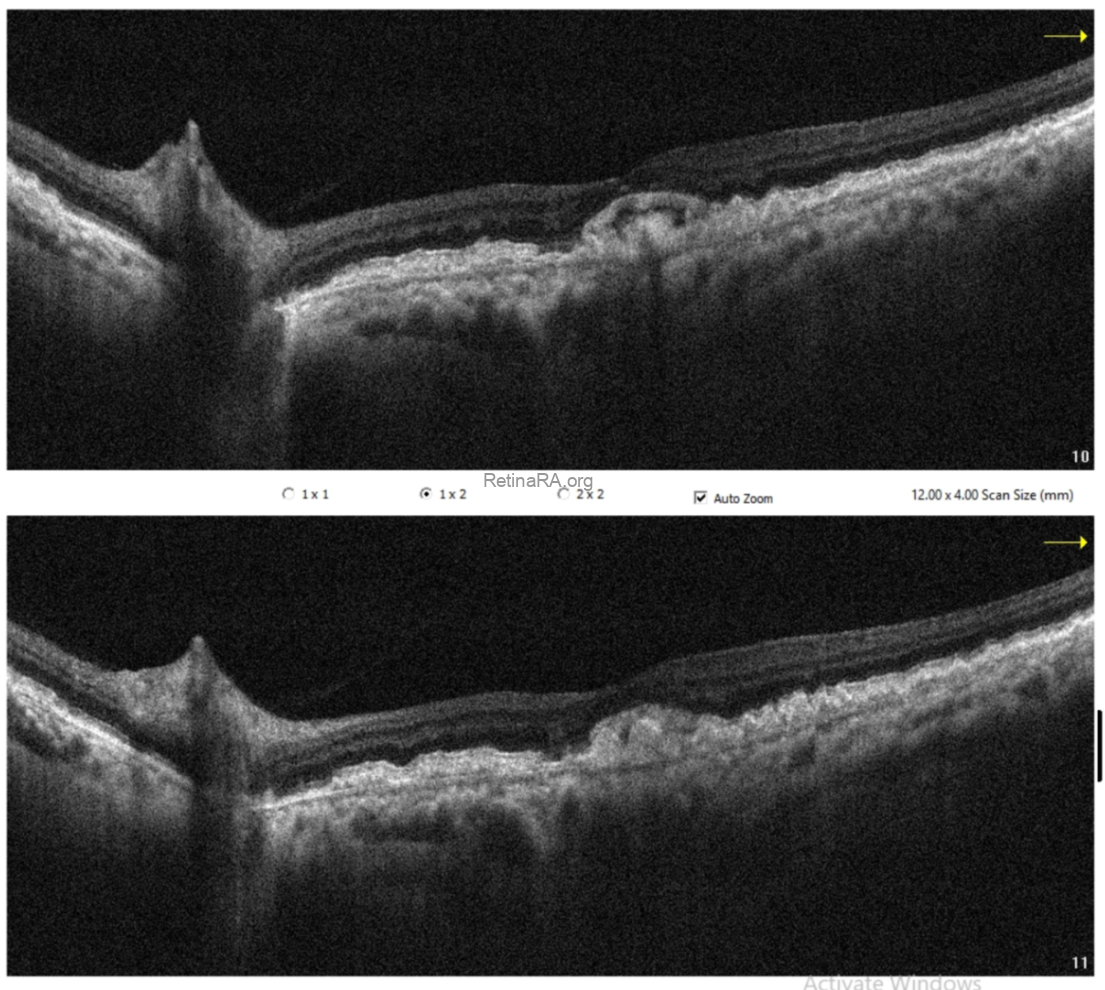
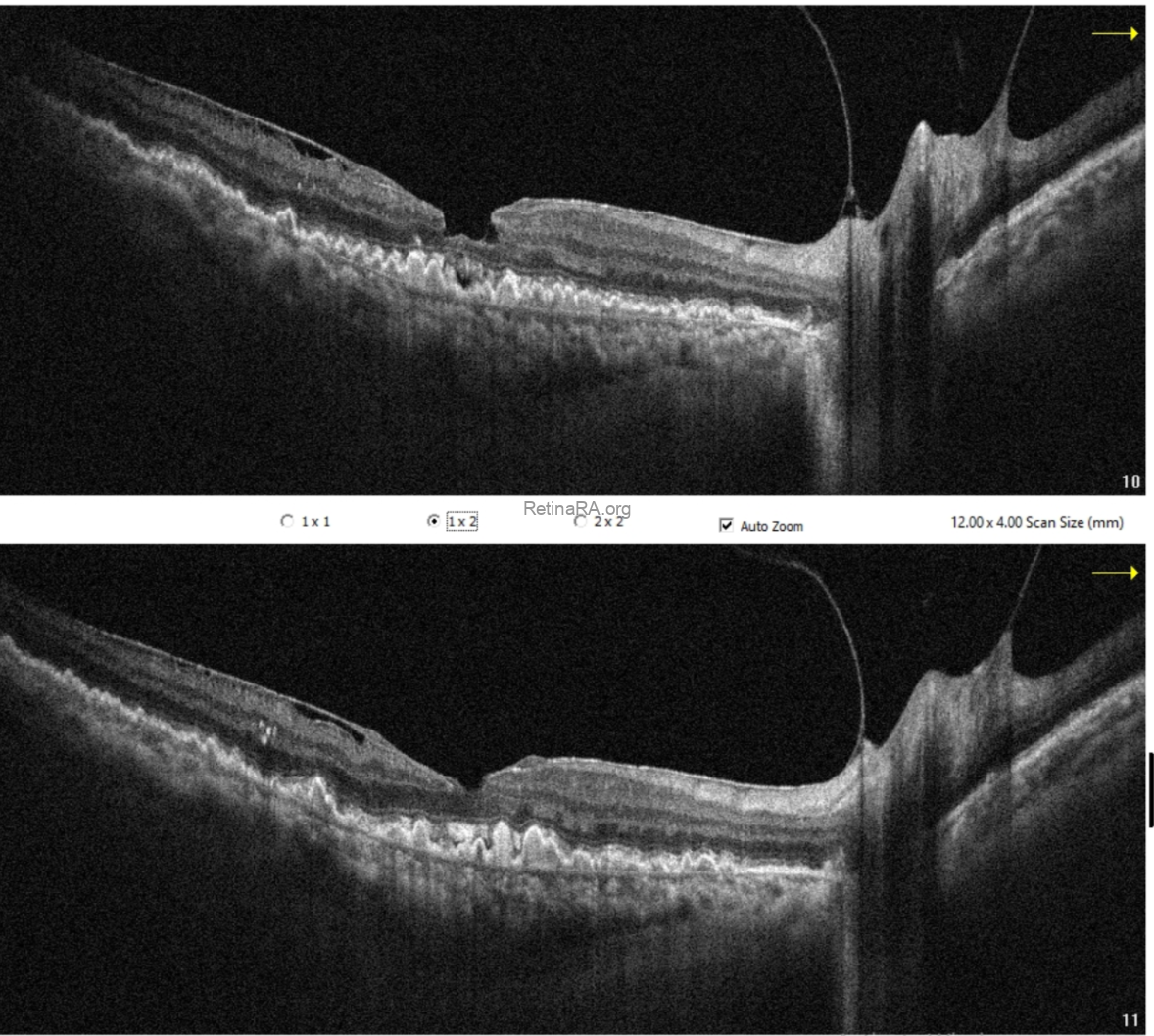
OCT angiography did not reveal any evidence of choroidal neovascularization. The subretinal fluid was therefore considered likely secondary to retinal pigment epithelium dysfunction.
Taking into account the patient’s systemic history, particularly membranoproliferative glomerulonephritis, these findings are consistent with dense deposit disease. This case highlights that, despite the patient’s advanced age, such presentations should not be attributed solely to age-related macular degeneration. A thorough evaluation of systemic associations is essential for accurate diagnosis.
Credit:
Case: Gunel Agayeva, Md
Badam Medical Center, Baku, Azerbaijan
Instagram account: @dr.gunel_agayeva_phd
Caption: M. Giray Ersoz, MD, FEBO
Memorial Hospital, Department of Ophthalmology, Istanbul, Turkey
Arel University School of Medicine, Department of Ophthalmology, Istanbul, Turkey
Instagram accounts: @retina.review and @retina.dr.girayersoz