A 44-year-old woman presented to the ophthalmology clinic for a routine eye examination. She was in good health, with no relevant ocular or medical history. Moderate myopia was noted in both eyes, and her best-corrected visual acuity was 20/20 bilaterally. Intraocular pressures were within normal limits, and the anterior segments appeared normal.
Fundus examination revealed a normal macula and optic disc in both eyes, with a relatively pale fundus.

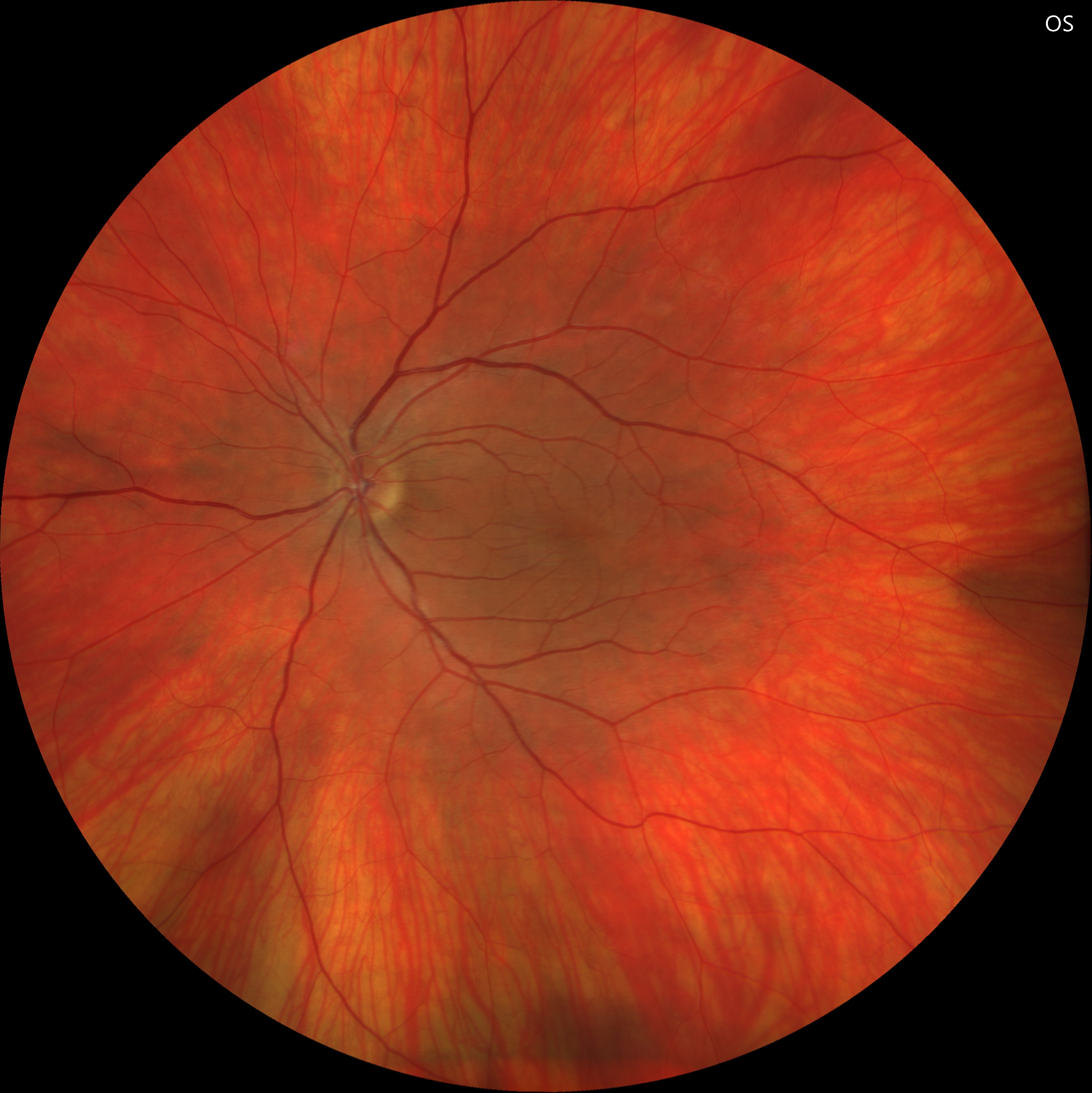
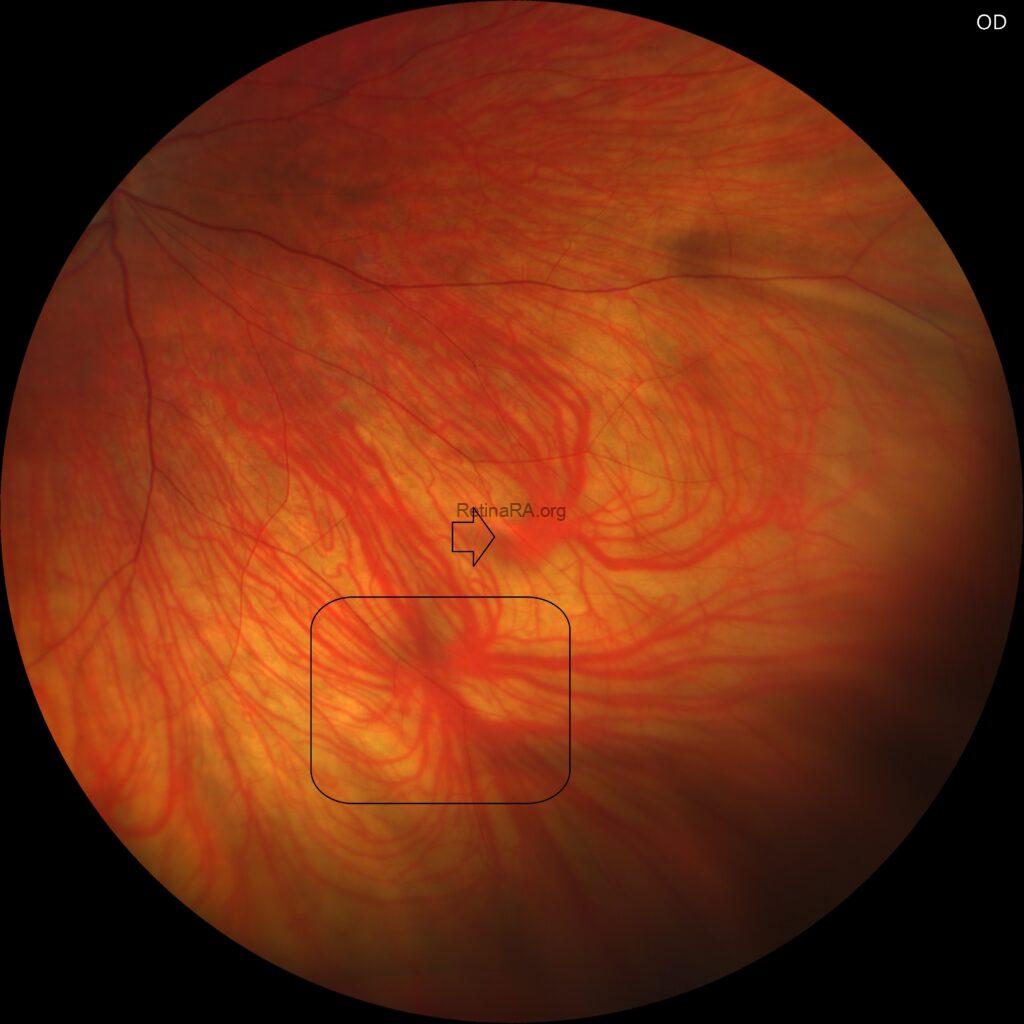
Midperipheral evaluation demonstrated prominent vortex veins with enlarged ampullae in both eyes.
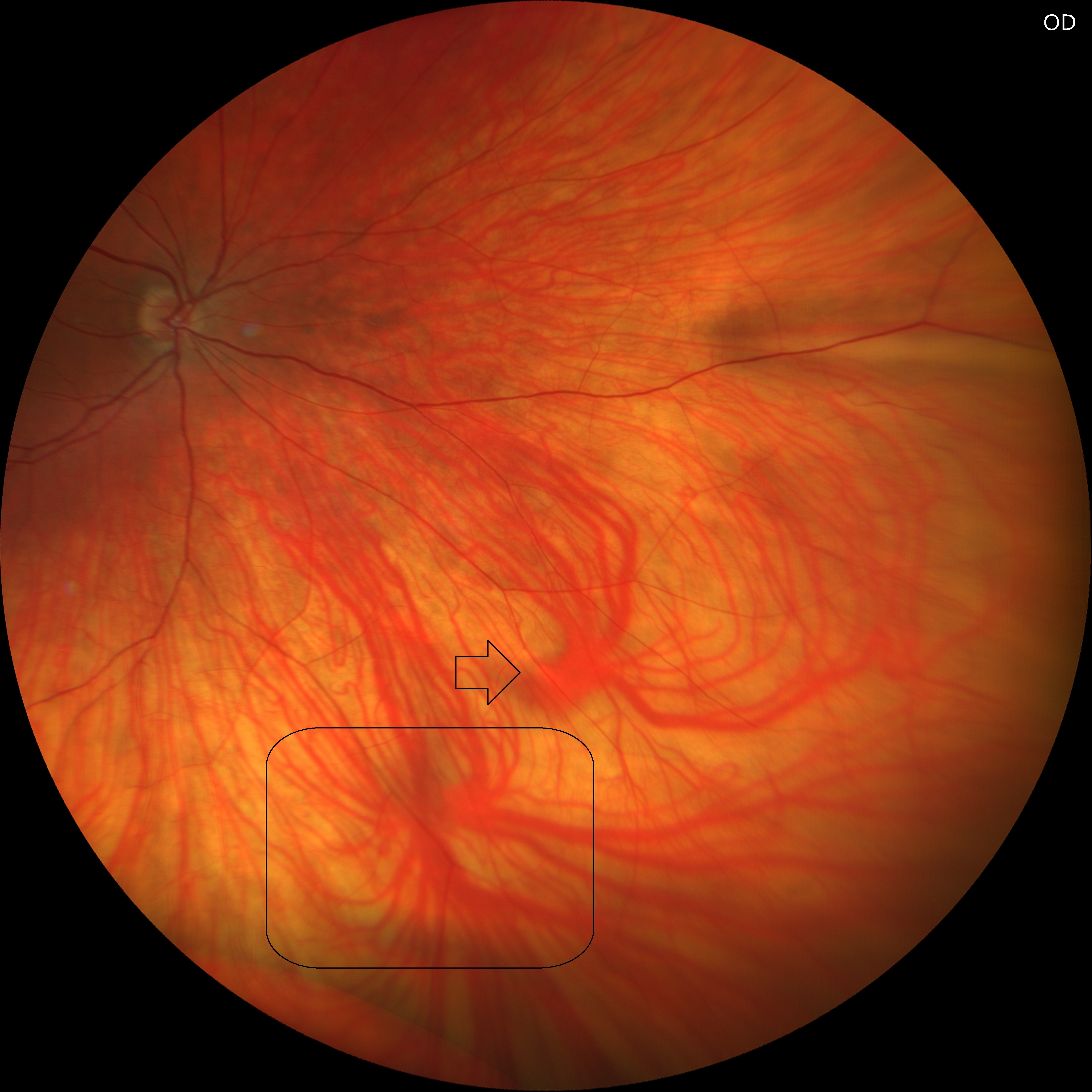
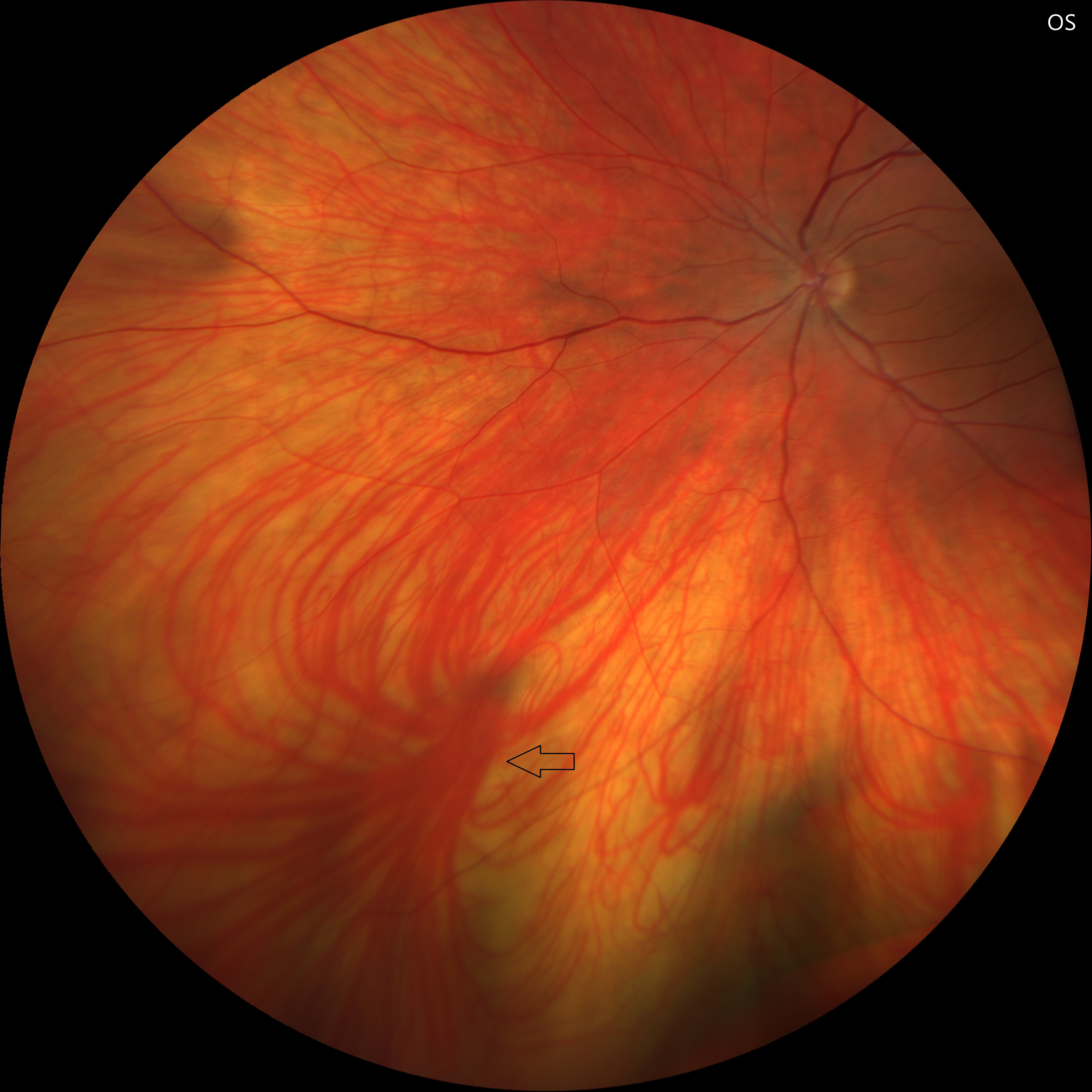

Vortex veins are major venous outflow pathways of the choroid, draining blood from the uveal tract into the ophthalmic veins. Typically, 4–8 vortex veins are located in each quadrant of the globe, converging at the equator. At this junction, each vortex vein forms a dilated segment known as the ampulla, which serves as a transitional site before the vein exits the sclera. These structures are clinically visible during fundus examination and can be highlighted with indocyanine green angiography. Alterations in vortex vein morphology, ampullary size, or drainage patterns have been implicated in various choroidal disorders, including pachychoroid spectrum diseases and central serous chorioretinopathy.