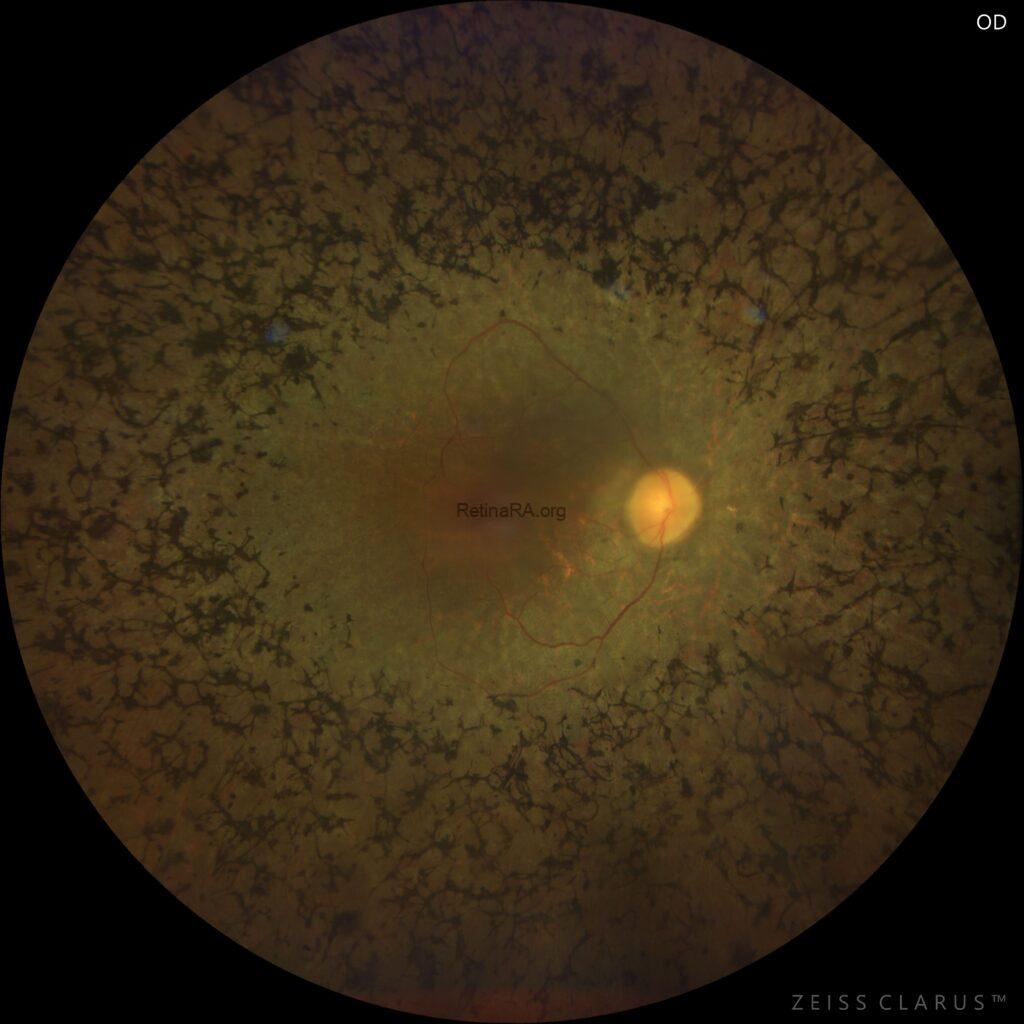
A 42-year-old male presented with progressive night blindness and peripheral visual field constriction, accompanied by recent worsening of central vision in both eyes. Family history was positive for similar visual complaints. Best-corrected visual acuity was 0.3 in the right eye and 0.4 in the left eye. Anterior segment examination was normal.
Color fundus examination revealed typical findings of retinitis pigmentosa, including mid-peripheral bone-spicule pigmentations, attenuated retinal vessels, waxy pallor of the optic disc, and diffuse retinal pigment epithelium atrophy with a mottled background. The macula showed a dull foveal reflex suggestive of macular involvement.
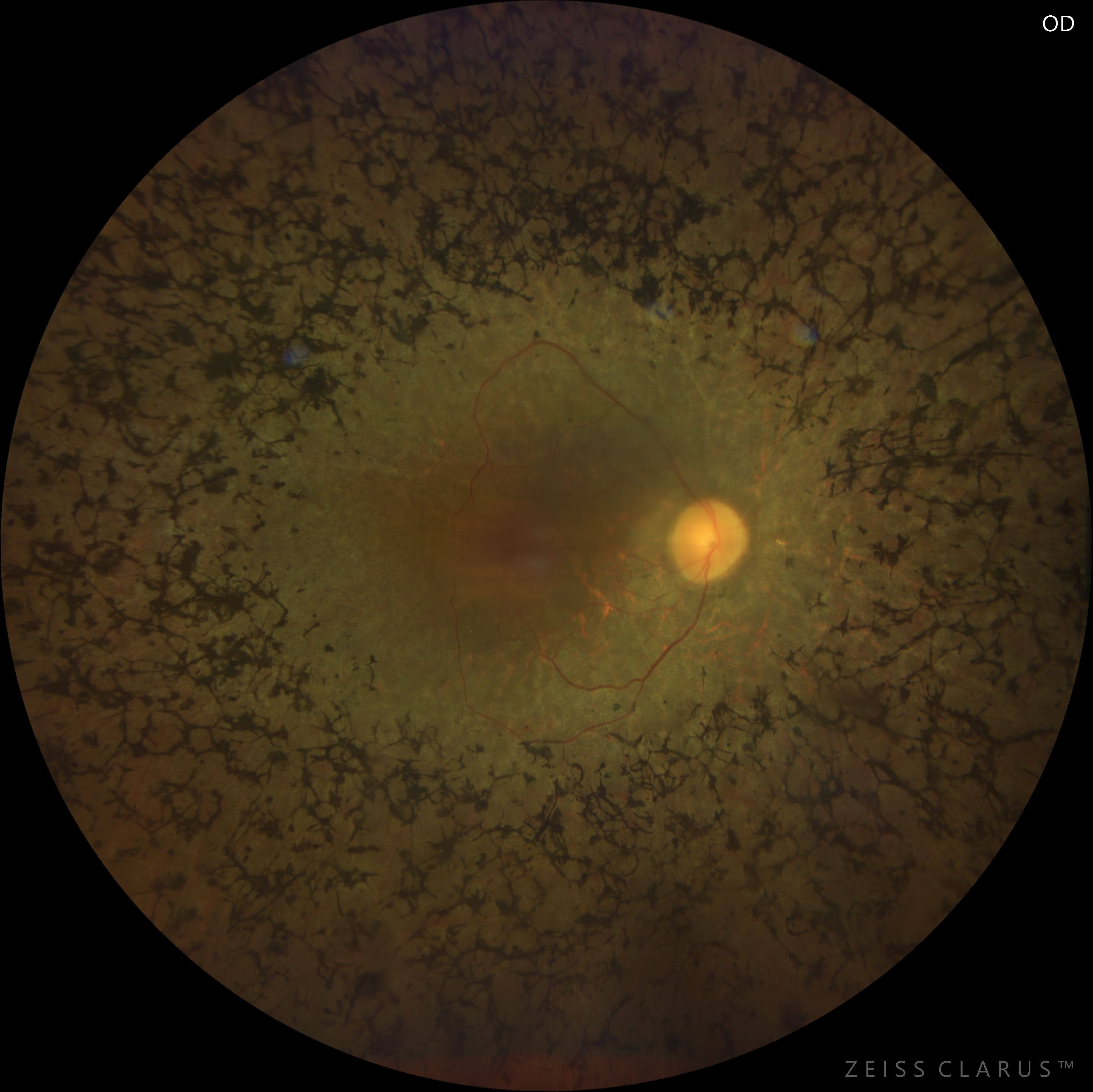
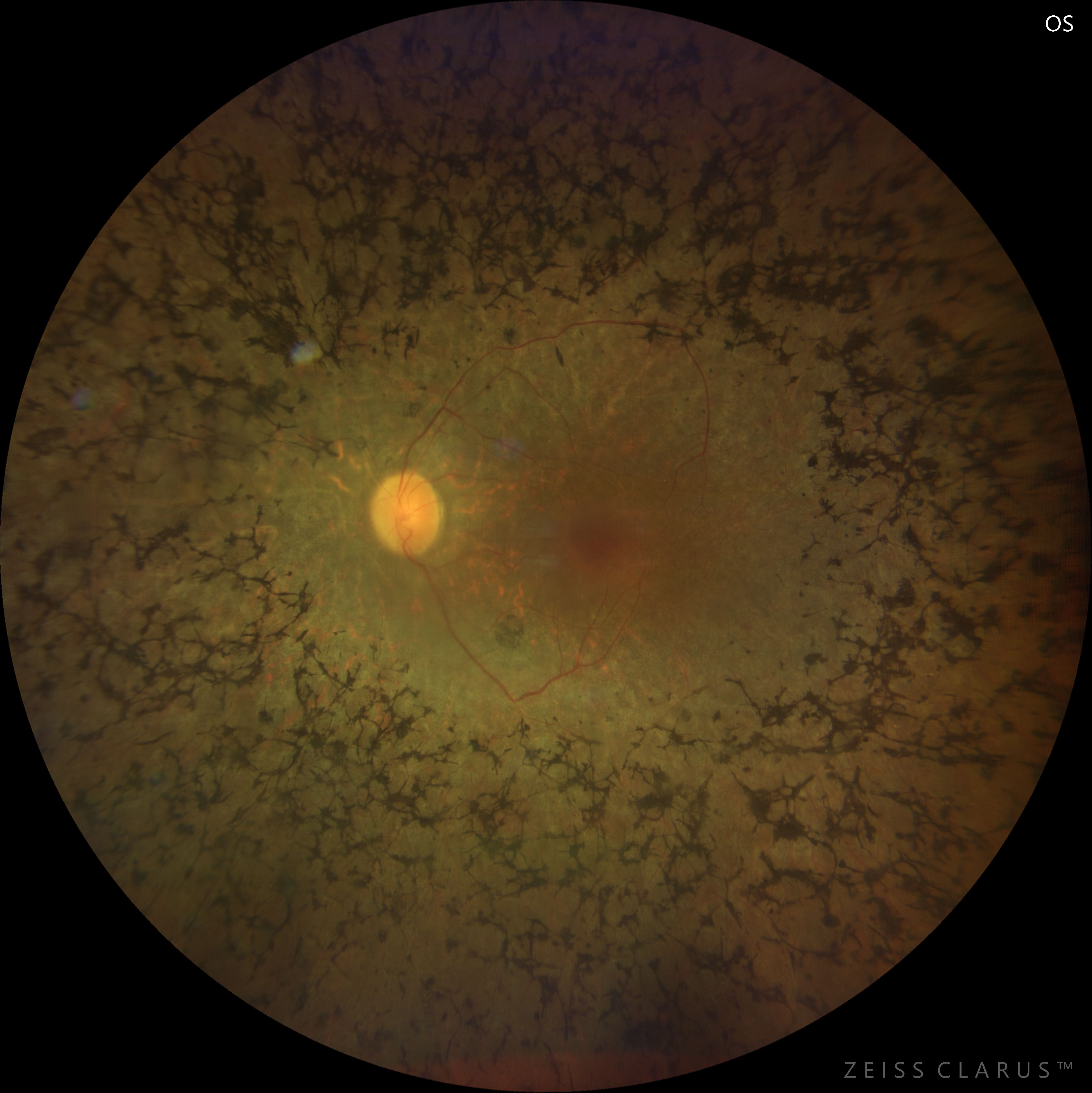
Spectral-domain optical coherence tomography of the macula demonstrated pronounced outer retinal atrophy, with disruption and loss of the ellipsoid zone. In addition, multiple intraretinal cystic spaces were present in the foveal and parafoveal regions, consistent with cystic macular edema. Structural alterations of the outer retina and the retinal pigment epithelium complex were also noted.
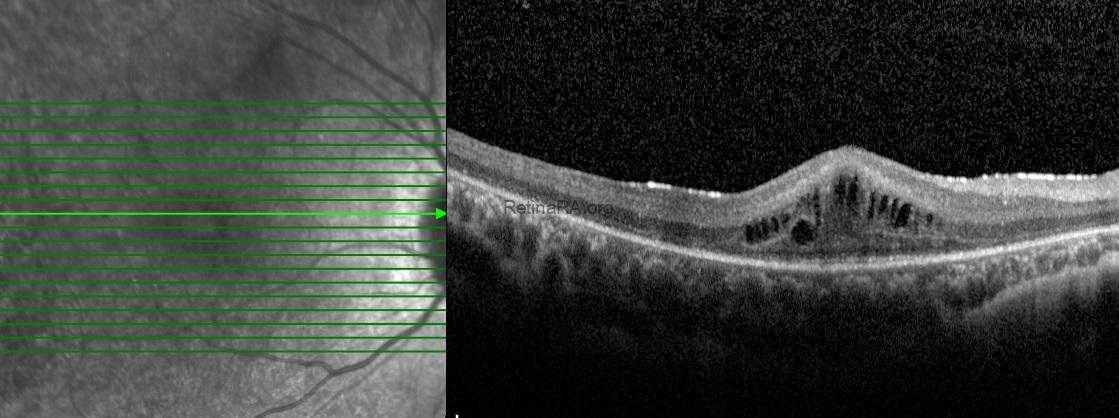
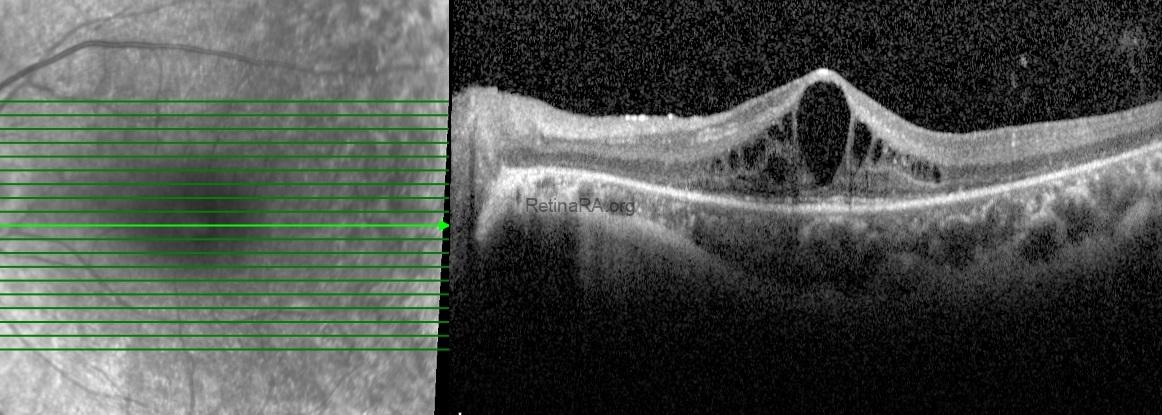
Based on the clinical and imaging findings, a diagnosis of retinitis pigmentosa with macular involvement was made. The coexistence of advanced outer retinal degeneration and cystic macular edema was considered the main contributing factor to the patient’s reduced central visual acuity.
Retinitis pigmentosa is a group of inherited retinal dystrophies characterized by progressive photoreceptor degeneration, primarily affecting rod cells in the early stages. Patients typically present with night blindness and gradual peripheral visual field loss, which may progress to central vision impairment in advanced disease. On fundus examination, classic findings include bone-spicule–like pigmentations in the mid-peripheral retina, attenuation of retinal vessels, and waxy pallor of the optic disc. Optical coherence tomography is essential for evaluating disease severity and macular involvement, often revealing outer retinal atrophy and disruption of the ellipsoid zone. Cystic macular edema is a common and potentially treatable complication that may significantly impact visual acuity. Although no curative treatment currently exists, early diagnosis, genetic counseling, and regular multimodal imaging are crucial for patient management. Advances in gene therapy and retinal prostheses continue to offer promising perspectives for selected patients with retinitis pigmentosa.
Credit: Kemal Tekin, M.D., from Ulucanlar Eye Training and Research Hospital
Instagram accounts: @retina.academy and @dr.kemaltekin